Urologic Diseases Information
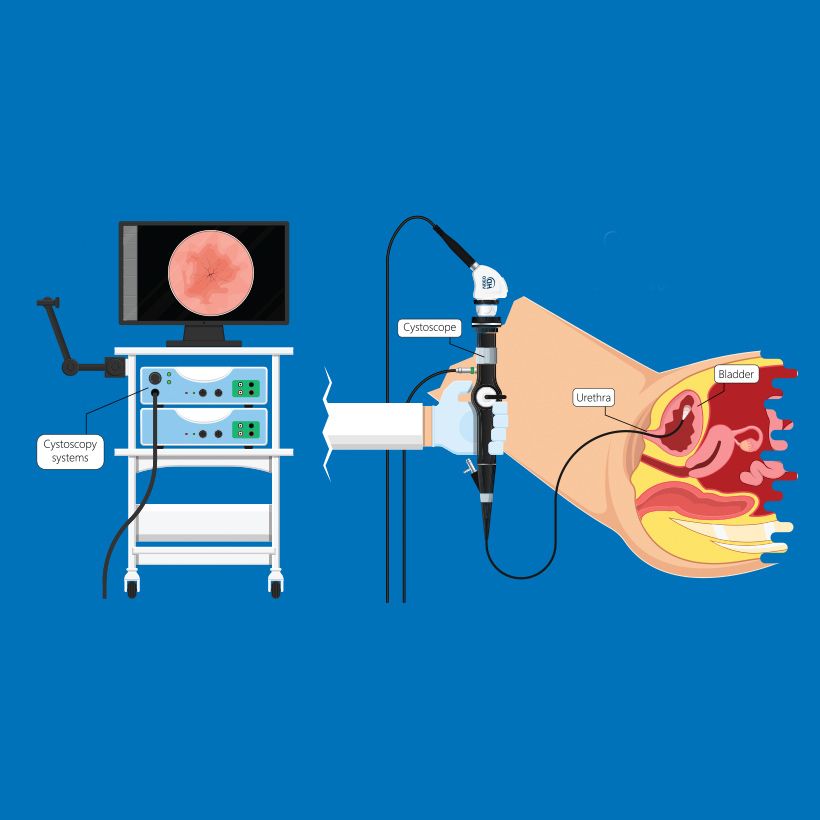
When you have a urinary problem, your doctor may use a cystoscope to see inside your bladder and urethra. The urethra is the tube that carries urine from the bladder to the outside of the body. The cystoscope has lenses like a telescope or microscope. These lenses let the doctor focus on the inner surfaces of the urinary tract. Some cystoscopes use optical fibers (flexible glass fibers) that carry an image from the tip of the instrument to a viewing piece at the other end. The cystoscope is as thin as a pencil and has a light at the tip. Many cystoscopes have extra tubes to guide other instruments for procedures to treat urinary problems. Your doctor may recommend cystoscopy for any of the following conditions:
frequent urinary tract infections
blood in your urine (hematuria)
unusual cells found in the urine sample
painful urination, chronic pelvic pain, or interstitial cystitis
urinary blockages such as prostate enlargement, stricture, or narrowing of the urinary tract
If you have a stone lodged in your ureter or have an area that needs more study in your ureter, your doctor may recommend a ureteroscopy, usually with general or regional anesthesia. The ureter is the tube that carries urine from the kidney to the bladder. The ureteroscope is a special, very thin instrument used to look directly at and visualize the inside of the ureter.
Some ureteroscopes are flexible like small, very long straws. Others are more rigid and firm. Through the ureteroscope, the doctor can see the stone. The doctor can then move the stone, either by removing it with a small basket at the end of a wire inserted through an extra tube in the ureteroscope or by extending a flexible fiber that carries a laser beam to break the stone into smaller pieces that can then pass out of the body in your urine. How and what the doctor will do is determined by the location, size, and composition of the stone. The doctor may leave a stent, a flexible tube that keeps the ureter open for drainage after the procedure.
Narrow Band Imaging Cystoscopy
Preparation
Ask your doctor about any special instructions. In most cases, you will be able to eat normally and return to normal activities after the test. Since any medical procedure has a small risk of injury, you will need to sign a consent form before the test. Do not hesitate to ask your doctor about any concerns you might have.
You may be asked to give a urine sample before the test to check for infection. Avoid urinating for an hour before this part of the test. You will wear a hospital gown for the examination, and the lower part of your body will be covered with a sterile drape. In most cases, you will lie on your back with your knees raised and apart. A nurse or technician will clean the area around your urethral opening and apply a local anesthetic.
If you are going to have a ureteroscopy, you may receive a spinal or general anesthetic. If you know this is the case, you will want to arrange a ride home after the test.
Test Procedures
The doctor will gently insert the tip of the cystoscope into your urethra and slowly glide it up into the bladder. Relaxing your pelvic muscles will help make this part of the test easier. A sterile liquid (water or saline) will flow through the cystoscope to slowly fill your bladder and stretch it so that the doctor has a better view of the bladder wall.
As your bladder reaches capacity, you will feel some discomfort and the urge to urinate. You will be able to empty your bladder as soon as the examination is over.
The time from insertion of the cystoscope to removal may be only a few minutes, or it may be longer if the doctor finds a stone and decides to remove it. Taking a biopsy (a small tissue sample for examination under a microscope) will also make the procedure last longer. In most cases, the entire examination, including preparation, will take about 15 to 20 minutes.
After the Test
You may have a mild burning feeling when you urinate, and you may see small amounts of blood in your urine. These problems should not last more than 24 hours. Tell your doctor if bleeding or pain is severe or if problems last more than a couple of days.
To relieve discomfort, drink two 8-ounce glasses of water each hour for 2 hours. Ask your doctor if you can take a warm bath to relieve the burning feeling. If not, you may be able to hold a warm, damp washcloth over the urethral opening.
Your doctor may give you an antibiotic to take for 1 or 2 days to prevent an infection. If you have signs of infection — including pain, chills, or fever — call your doctor.
Cysto With Stents
General
DIET:
No restrictions on diet, drink at least 8-10 oz. Glasses of fluid every day, unless restricted by your physician. Avoid caffeine. Try water with lemon wedges, soup, 7-up.
NAUSEA:
There may be some nausea after your anesthesia. If nausea is present, rest in bed. After nausea has stopped try fluids such as listed above.
DISCOMFORT:
The amount of discomfort is very unpredictable. You may have some burning upon voiding, blood-tinged urine, and urinary frequency. It is not uncommon to have spasms (colicy or intermittent pain, pain that comes and goes) of the ureter (flank area) or urethra (bladder) while the stent is in place. For pain relief and promotion of muscle relaxation, take a warm bath or apply heat to the abdomen. Unless contraindicated take Tylenol for the discomfort, according to package directions.
BLEEDING:
It is not uncommon to pass blood or small clots, especially the first 72 hours. Keep drinking fluids.
FEVER:
A low-grade fever is common even after a simple procedure. If your temperature is elevated, drink plenty of fluids. If you have questions about your temperature, do not hesitate to notify your doctor.
ACTIVITY:
We suggest resting as much as possible the day of surgery, then you may resume your normal activity as you feel like it. Do not drive a car for 24 hours after a general anesthetic. You may experience some blood in your urine with increased activity, such as lifting, exercising, or sexual intercourse, with a stent in place. This is normal, continue to drink plenty of fluids.
EMERGENCY CALLS:
If you have a problem of an emergency nature and are unable to reach your doctor, come to your nearest hospital or emergency facility. If unable to pass your urine, first try sitting in a warm tub and void, if still unable to void go to the nearest Emergency Outpatient Department.
Contact your doctor (or doctor on call) if you have any problems:
• Fever over 100 oral
• If the stent is coming out of the urethra and was not placed there at the time of surgery.
• Large amount of bright blood or clots in urine.
• Pain unrelieved by medication or warm bath.
• If burning upon urination, frequency and blood in urine continues after 72 hours post-op.
• If it is necessary for you to contact your doctor before your office visit, he can be reached at his office number.